Introduction Norovirus on Food
 At the 2017 World Athletics Championships, Botswana sprinter Isaac Makwala qualified for the 200m semi-finals in a quite unusual way: by running the heat – and celebrating afterwards – all alone.
At the 2017 World Athletics Championships, Botswana sprinter Isaac Makwala qualified for the 200m semi-finals in a quite unusual way: by running the heat – and celebrating afterwards – all alone.
During that week, Makwala, along with other athletes, had been infected by Norovirus as a result of food poisoning, which supposedly originated in the hotel where they were staying,
When the runner showed up for the scheduled qualifying heat, he was obviously feeling fit enough to compete, but the judges decided to keep him out of the stadium nonetheless, for fear of him infecting other athletes.
In the end, all went well for Makwala, who qualified for the final on the same day as his solo race, running with the rest of the group. However, the IAAF was severely criticized for not allowing him to run with the rest of the sprinters. After all – such was the reasoning of notable commentators – the fact that he showed up to run could only mean that he had fully recovered, so there was no reason for keeping him away.
The IAAF’s decision was, in fact, irreproachable: the first 48 hours after the disappearance of symptoms is when a person affected by Norovirus is more likely to spread the infection. If anything, the ensuing criticism was a good demonstration of the general lack of awareness around this illness.
Unfortunately, this lack of awareness extends to the food industry, where Noroviruses tend to be underestimated, and too often there are no effective practices in place to prevent contamination.
What is Norovirus?
 Norovirus (also called Norwalk virus, from a city in Ohio where an outbreak occurred in 1968) causes attacks of acute gastroenteritis with its typical symptoms being nausea, vomiting, diarrhea and abdominal cramps. The incubation period is between 12 and 48 hours (33 hours on average) and symptoms last between 24 and 60 hours. The virus is transmitted through feces and vomit, either directly from person to person, or via contaminated water, air and food.
Norovirus (also called Norwalk virus, from a city in Ohio where an outbreak occurred in 1968) causes attacks of acute gastroenteritis with its typical symptoms being nausea, vomiting, diarrhea and abdominal cramps. The incubation period is between 12 and 48 hours (33 hours on average) and symptoms last between 24 and 60 hours. The virus is transmitted through feces and vomit, either directly from person to person, or via contaminated water, air and food.
There are different types of Noroviruses, and some of them are more associated with foodborne infections than others. Although it’s destroyed by heat, it can survive temperatures up to 60°C / 140°F and as few as 18 particles can be enough to cause an infection. As a consequence, it can spread fast and easily. The outbreak at the World Athletics Championships shows how not even a group of professional athletes staying at a four-star hotel in London were immune to it.
Norovirus outbreaks are more frequent during the winter, when people spend more time indoors. For that reason, it’s usually called “winter vomiting bug” in the UK and Ireland. Although it’s not the only cause of acute gastroenteritis, it’s estimated that it contributes to 60% of worldwide cases, and that 14% of them are foodborne.
Few deaths, high impact
Data on food safety incidents shows that, while bacteria-related illnesses such as Salmonella, E.coli and Listeria cause more deaths and deserve all the attention they get, Noroviruses are not deemed as critical. A comparison between Norovirus and Salmonella will help shed some light on the different attitudes of the food industry about their respective food safety issues.
According to the RASFF database, which keeps track of all food incidents since 2001, in 2015 there were 953 Salmonella-related incidents, 91 of them were reported following the company’s own checks. On the other hand, the same thing happened for only 2 Norovirus cases out of 289, which were reported in the RASSF database. The difference is 9.55% vs 0.69% of outbreaks being notified by the producer itself.
This difference in reporting and alertness most likely stems from the assumptions that Noroviruses are not so dangerous after all and that it’s relatively easy to deal with them.
An infection with a Norovirus is not lethal per se, although it can cause complications in vulnerable patients like small children, the elderly, or people with existing medical conditions. On the other hand, data elaborated by the EFSA on food incidents in 2015 shows that Salmonella poses a greater risk to people’s health. In 2015, Salmonella alone accounted for 1719 hospitalizations and 3 deaths, while Norovirus caused 352 hospitalizations and 1 death.
However, even when a medical condition won’t cause as many deaths, it still has a social cost, especially when it involves a high number of subjects.
With that respect, data confirms how Norovirus can spread much faster than Salmonella. While the typical Norovirus outbreak involves 46.8 people on average, a Salmonella outbreak only involves 6.9 people.
Additionally, reported food incidents don’t tell the whole story of the real impact that foodborne illnesses have on society. Although the EU food system is very good at investigating real or potential risks and taking countermeasures, the food recall system has its limitations. First of all, many foodborne contaminations are asymptomatic. With Norovirus, these can be up to 30%. Of course, the virus can be transmitted even in the absence of symptoms.
Secondly, the incubation period makes it difficult to associate foodborne illnesses to a specific food. Even when an outbreak can be traced back to a specific location, it might still be impossible to find out exactly what foodstuff caused it.
For example, a recent case of Norovirus outbreak in Ohio was connected to a local coffee shop. However, after two weeks of investigation, local authorities had to admit that they may never know the real source of the virus.
Killing the Norovirus in food with heat is not enough
 The second assumption, which may generate a false sense of security around Noroviruses, is that occurrences can be easily prevented. Because sterilizing, pasteurizing, or cooking at high enough temperatures effectively kills the virus, a lot of processed food is supposed to be safe from Norovirus contamination, which would leave us with fresh, unprocessed food as the main offender.
The second assumption, which may generate a false sense of security around Noroviruses, is that occurrences can be easily prevented. Because sterilizing, pasteurizing, or cooking at high enough temperatures effectively kills the virus, a lot of processed food is supposed to be safe from Norovirus contamination, which would leave us with fresh, unprocessed food as the main offender.
All that is true and supported by data. According to the RASFF database, raw or undercooked shellfish – especially oysters – is mainly responsible for Norovirus outbreaks. The list also includes lettuce and berries. For example, a large outbreak that occurred in 2012 in Germany, affecting more than 11,000 young children, was caused by frozen strawberries from China.
However, using heat to kill the virus only eliminates one contamination channel. Norovirus infections can also be airborne or happen through direct contact, either in a food factory or at the point of use (e.g. restaurant or home kitchen). In some instances, temperature-treated food stuff might still be prone to post contamination via human carriers of the Norovirus in the (high care) processing area.
The three elements of an effective prevention policy
Because Noroviruses cause a quite infectious illness with a high impact on society, the food industry should do more to create safe processing environments.
Company culture comes first

This Thursday, Jan. 12, 2017, photo, shows the sign on a Chipotle restaurant in Pittsburgh. Chipotle Mexican Grill, Inc. reports financial results, Tuesday, July 25, 2017. (AP Photo/Gene J. Puskar)
In 2015, the reputation of American burrito chain Chipotle was seriously damaged by a severe outbreak of E.coli that started from their restaurants. In July this year, the fast food chain was responsible for another outbreak, this time of Norovirus. As the company confirmed, it originated from an employee who caught the virus but came to work anyway. In spite of all the improvements to their food safety practices after the first incident, Chipotle apparently neglected to enforce their sick leave policy with store managers.
Doctors’ indications are very clear in these instances: Norovirus is most contagious at least during the first 48 hours after symptoms disappear. Just like Makwala was kept away from the track for two days after his recovery, food workers should not be allowed to come back to work as soon as they feel good enough. Unfortunately, actual industry practices go too often in the opposite direction.
Clear company policies are essential but, as the Chipotle example shows, rules are of little use if there’s no real determination to enforce them. That’s why preventing Noroviruses in the food industry is first of all a matter of company culture and awareness.
Hygiene and sanitation practices
Thorough hand washing is the single most effective sanitation practice against Norovirus contamination. “Thorough” means that a quick wash with a hand-sanitizer won’t do. At least 30 seconds of intense rubbing is necessary to effectively clean hands. Of course, after properly washing the hands, a sanitizer must be applied to get rid of any potential remaining viruses and harmful bacteria.
Also, whenever a food operator shows symptoms during work, he or she should be sent home immediately on sick leave. The next step will be to sanitize all surfaces that food operator may have touched, including toilets. The virus tends to be quite resistant to cleaning agents, but a chlorine bleach solution proved to be most effective.
Environmental monitoring
Good hygiene practices are necessary but not enough. Too often, food operators do not actively look for the presence of Noroviruses in their factory environment.
Whereas it is common practice to check for the presence of (pathogenic) bacteria close to food contact surfaces and in the wider factory environment on a structural basis, testing for Noroviruses is hardly performed in the international food industry. Nowadays there are good PCR or ELISA tests kits available to effectively test for the presence of Noroviruses.
As indicated earlier, a Norovirus outbreak is more likely to happen during winter, hence the environmental monitoring on the presence of Noroviruses should be intensified during that period. Monitoring should be executed during and after any suspected Norovirus-related illness occurrence involving one or more of the employees working in a food factory. This must include the office staff as well, as these might use the same facilities as the people working with foodstuff that is exposed to the air.
Conclusion can Norovirus live in food
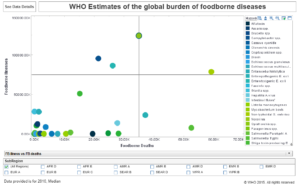 As shown in a study performed by the World Health Organization based on endemic data gathered across the globe, Norovirus outbreaks represent a significant part of the overall load of foodborne illnesses and even foodborne-related deaths.
As shown in a study performed by the World Health Organization based on endemic data gathered across the globe, Norovirus outbreaks represent a significant part of the overall load of foodborne illnesses and even foodborne-related deaths.
The global food producing and processing industries should pay more attention to the preventive measures in relation to Noroviruses. Proper hand hygiene, the right company mentality in the case of employees falling ill, ensuring that the sick leave is extended for at least 48 hours after recovery, and the inclusion of Noroviruses in the environmental monitoring program are crucial factors in the reduction of Norovirus outbreaks.
Additional blogs:
5 Secrets to Prevent Salmonella from Ending up in Your Product
Workshop Personal Hygiene Management